|
Get AfricaFocus Bulletin by e-mail!
Format for print or mobile
Africa/Global: People's Vaccine vs. Vaccine Apartheid
AfricaFocus Bulletin
April 6, 2021 (2021-04-06 )
(Reposted from sources cited below)
Editor's Note
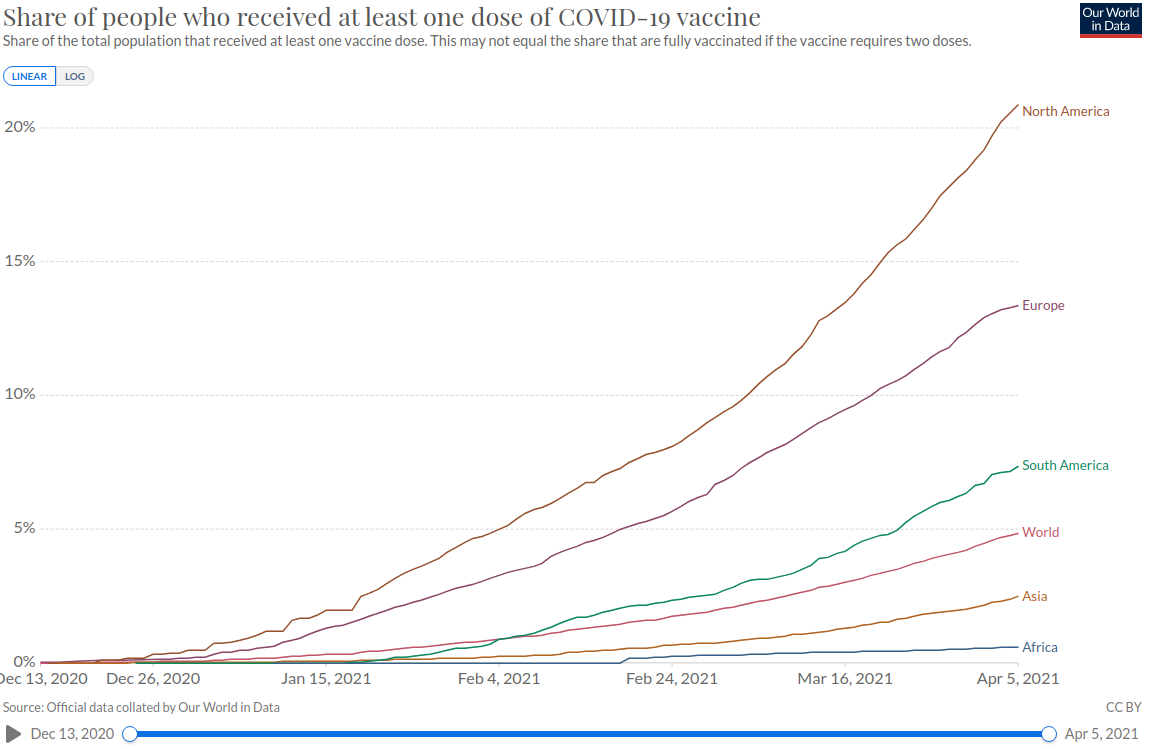
Despite the vast disparity in the pace of vaccinations for Covid-19, currently at over 20% having one dose in North America, 5% in the world, and less in 1% for Africa, the United States, other rich countries, and pharmaceutical companies are still rejecting growing demands to waive patents and transfer technology. See chart below and data by country at https://ourworldindata.org/covid-vaccinations.
�In prepared remarks Monday [April 5] to the Chicago Council on Global Affairs ahead of meetings this week of international finance officials,� according to the Washington Post, Yellen called on richer countries to step up both economic and public health assistance to poorer nations reeling from covid. She noted as many as 150 million people across the world risk falling into extreme poverty as a result of the crisis.�
�This would be a profound economic tragedy for those countries, one
we should care about. But, that�s obvious. What�s less obvious � but
equally true � is that this divergence would also be a problem for
America," Yellen said. �Our first task must clearly be stopping the
virus by ensuring that vaccinations, testing and therapeutics are
available as widely as possible."
[The full speech, in which Yellen also called for international agreement on a global minimum corporate tax, is available on YouTube at https://www.youtube.com/watch?v=eR-2jA1gtOQ
This AfricaFocus includes several recent articles and other links
documenting the potential to begin to repair this wide gap. The major
barrier is political will on the part of those forces still trying to
monopolize vaccinations and profits for themselves.
For previous AfricaFocus Bulletins on Africa's health, visit
http://www.africafocus.org/intro-health.php
For an article on vaccination from January this year, see http://www.africafocus.org/docs21/vacc2101.php
For a March 25, 2021 Zoom webinar on Covid-19 Vaccines for Africa and her diaspora
Africans Rising, Advocacy Network for Africa, and Africa and African Diaspora
https://fb.watch/4BpZ91RWOb/
Includes updates from the Africa CDC on current status and a wide range of well-informed speakers.
For a global petition, now at almost 1 million signatures, visit
https://secure.avaaz.org/campaign/en/peoples_vaccine_2021_loc/
For petitions to the U.S. Congress and to President Biden, visit
https://www.oxfamamerica.org/explore/emergencies/covid-19-peoples-vaccine/,
https://sign.moveon.org/petitions/support-the-people-s-vaccine-1
or�https://rethinktrade.org/actions/urge-biden-reverse-trumps-deadly-obstruction-of-global-covid-19-vaccine-access/
+++++++++++++++++++++++++++++++++++++++++++++++++++
|
Webinar on April 12, 2021

Register at https://tinyurl.com/3b2erv5a
++++++++++++++++++++++end editor's note+++++++++++++++++
Coalition Calls on Biden to Use US-Owned Patent to Share Covid Vaccine With the World
"The U.S. government can help end the pandemic if it uses its legal leverage with Moderna to jumpstart an ambitious vaccine manufacturing program to benefit the world."
Common Dreams, March 26, 2021
by Jake Johnson, staff writer
https://www.commondreams.org/news/2021/03/26/coalition-calls-biden-use-us-owned-patent-share-covid-vaccine-world
Public health advocacy groups and scientists are pressuring the Biden administration to use the U.S. government's�ownership�of a key patent as leverage to ensure that the coronavirus vaccine�co-developed�by Moderna and National Institutes of Health is widely produced and distributed around the world, particularly in developing countries.
The patent in question covers crucial spike-protein technology�developed�by the NIH, an invention that has since been utilized in�at least five major�Covid vaccines�including�the Moderna-NIH shot formally known as mRNA-1273.
In a�letter�(pdf) earlier this week to Health and Human Services Secretary Xavier Becerra, NIH Director Francis Collins, and National Institute of Allergy and Infectious Disease Director Anthony Fauci, a coalition of advocacy groups led by�PrEP4All�and around a dozen scientists said the government-owned patent should be used as a "tool" to "facilitate scale-up of production of mRNA-1273 and ensure rapid, equitable global access."
"The U.S. government has not licensed the patent to Moderna. It is
imperative that the NIH uses any licensing agreement to include
provisions to help increase global access to this lifesaving
technology, rather than just a monetary royalty," the letter reads.
"U.S. taxpayers have invested over $2.5 billion in the development of
mRNA-1273. Now it is time for our government to ensure that this
critical lifesaving technology be made available to all. This could
contribute to saving millions of lives globally."
The new demand comes as the United States and other rich nations continue to block an India and South Africa-led push to temporarily waive certain international patent protections in order to expand access to coronavirus vaccines in countries currently�struggling to administer a single shot.
In their letter on Wednesday, the public health organizations urged
the U.S. government to use its leverage to negotiate patent licensing
terms that "require technology sharing with the World Health
Organization to help ramp up global production" and guarantee
widespread distribution of the vaccine at a low cost.
As the�New York Times�reported�earlier this week, the WHO "created a technology pool last year to encourage companies to share know-how with manufacturers in lower-income nations. Not a single vaccine company has signed up."
"The problem is that the companies don't want to do it," James Love,
head of the nonprofit Knowledge Ecology International, told the
Times. "And the government is just not very tough with the
companies."
Peter Maybarduk, director of the Access to Medicines program at
Public Citizen, lamented in a statement that "the U.S. government has
an embarrassing history of giving away publicly-funded and publicly-
owned medical technology to corporations, which then ration it back
to the people at monopoly prices."
"The U.S. government can help end the pandemic if it uses its legal
leverage with Moderna to jumpstart an ambitious vaccine manufacturing
program to benefit the world," Maybarduk said. "We must do better.
Many lives are at stake."
Read the full letter:
Dear Secretary Becerra, Dr. Collins, and Dr. Fauci:
We write about the soon-to-issue-patent, U.S. Patent No. 10,960,070
("the '070 patent"), that protects the use of proline-substituted
coronavirus spike proteins stabilized in their prefusion conformation
as a vaccine immunogen. The mRNA-1273 vaccine, co-developed by NIAID
and Moderna, utilizes this technology for its immunogen. The '070
patent is owned by the United States Government, reflecting the
critical contributions that NIAID and NIH made to the invention of
this technology.
This government-owned patent is an important policy tool that the
U.S. government could use to facilitate scale-up of production of
mRNA-1273 and ensure rapid, equitable global access. Currently, at
best, only one billion doses of mRNA-1273 will be produced in 2021,
far short of global demand.
The U.S. government has not licensed the patent to Moderna. It is
imperative that the NIH uses any licensing agreement to include
provisions to help increase global access to this lifesaving
technology, rather than just a monetary royalty.
Specifically, the licensing agreement should:
1. Empower the U.S. government to authorize manufacturing of
mRNA-1273�including by government-owned production facilities.
Currently, Moderna has only contracted with a single contract
manufacturing organization (CMO), Lonza Group AG, to produce drug
substance for mRNA-1273. By contracting with other CMOs to produce
drug substance and help perform other manufacturing steps, more doses
of mRNA-1273 could be produced. Such provisions should include the
ability for the U.S. government to compel transfer of know-how from
Moderna to other CMOs to facilitate scale up for all production steps
of the manufacturing process.
2. Require technology sharing with the World Health Organization to
help ramp up global production.
The Director-General of the World Health Organization has urged
countries to share vaccine technology and know-how openly to help
build global manufacturing capacity. Moderna has so far ignored
requests from developing country manufacturers to share technology.
Requiring Moderna to work with the WHO's COVID-19 technology access
pool can help unlock additional production.
3. Include requirements for accessible pricing universally.
Moderna is currently charging between US$10 and US$40 a dose for
mRNA-12738, despite it costing less than $3 a dose to manufacture.
This high price, coupled with Moderna's lack of planned market entry
for many low-and middle-income countries, may prevent those most in
need from accessing mRNA-1273. Licensing the '070 patent gives the
U.S. government leverage to increase global access by requiring
accessible pricing to mRNA-1273.
Assertion of U.S. government-owned intellectual property to increase
access to pharmaceutical products is not unprecedented. In 2019, the
federal government sued Gilead Sciences for its infringement of
government owned patents protecting the use of Truvada and Descovy
for HIV pre-exposure prophylaxis (PrEP)�and per the complaint itself,
is using that litigation to increase access to PrEP. That lawsuit is
ongoing.
U.S. taxpayers have invested over $2.5 billion in the development of
mRNA-1273. Now it is time for our government to ensure that this
critical lifesaving technology be made available to all. This could
contribute to saving millions of lives globally. It also will help
protect public health here at home. Global vaccination with highly
effective vaccines, like mRNA-1273, is our best defense against the
development of vaccine-resistant variants of SARS-CoV2.
Thank you.
**************************************************************
U.S. and European COVID-19 shots aren�t enough. It is time to tap
into Africa, Asia, and Latin America�s enormous production capacity.
by Matthew Kavanagh, Mara Pillinger, Renu Singh, Katherine Ginsbach |
March 1, 2021
[Excerpt: for full article visit
https://foreignpolicy.com/2021/03/01/to-democratize-vaccine-access-democratize-production/
As wealthy countries inoculate millions of their citizens against
COVID-19 and other countries wait to even begin the rollout, G-7
leaders are increasingly struggling to address geopolitically charged
vaccine inequities.
French President Emmanuel Macron recently noted his fear that
countries would turn to China and Russia for vaccines and �the power
of the West will ... not be a reality.� He later walked back his
statement somewhat, clarifying that vaccines are a matter of public
health�not power. They are, of course, both. But Macron and other
leaders will never get either issue right as long as they remain
focused on what portion of a relatively small supply of vaccines to
share. Rather, the real game-changer lies in a very feasible effort
to expand the pool of available vaccines.
At the moment, vaccine production approved in the United States and
Europe is needlessly limited to a handful of companies struggling to
get enough vaccines out the door to meet demand. Yet in Africa, Asia,
and Latin America, there is enormous human and production capacity
that could be mobilized to make more vaccines and address the needs
of people in low- and middle-income countries. Governments and
companies, especially in middle-income countries, have been asking to
do so. As Western firms have demurred, Russia has taken them up on
their offers, sharing Sputnik V know-how for production in Brazil,
India, Turkey, and South Korea. If U.S. and European Union leaders
want to address both the public health and diplomatic imperatives
facing them�while also vaccinating their own populations�they should
consider doing the same.
Vaccine development is largely funded by public money. The United
States and Europe have poured massive resources into research and
development as well as advance purchase agreements that remove risks
for companies to develop vaccines. The United States, for example,
put $2.48 billion into the new National Institutes of Health (NIH)
/Moderna vaccine alongside a huge investment of effort in government
scientists who pioneered them. Likewise, the German government
provided $445 million to develop the Pfizer-BioNTech vaccine.
This spending brought remarkable breakthroughs for stopping COVID-19
and for future global health security. The kinds of shots Moderna,
Pfizer-BioNTech, and others have developed are messenger RNA (mRNA)
vaccines, which are simpler to make, easier to scale, and faster to
adapt in the face of variants than traditional vaccines. The
technology might soon bring breakthroughs against HIV, malaria, or
influenza and enable rapid COVID-19 vaccine development against new
emerging diseases. Logistical challenges that have dogged the
deployment of COVID-19 vaccines, like cold chain storage, can be
tackled. Moderna, for example, announced just before approval that
its vaccine can now be kept refrigerated, not frozen, for 30 days.
The United States and Europe have far more to gain by sharing these
technologies than by hoarding them, from preventing a never-ending
cycle of new variants to rebuilding global trade and gaining soft-
power influence. They should immediately work to allow production of
cutting-edge COVID-19 vaccines in Africa, Asia, and Latin America.
Some observers have claimed that such an effort would not be
possible, take too long, or cost too much. They are wrong, as the
world�s experience developing HIV medicines shows.
After millions died without access to medications, today�s cutting-
edge HIV drugs frequently come to market with near-simultaneous
production by multiple companies in low- and middle-income countries.
This is a direct result of government investment in production
capacity, sharing of technology, and use of voluntary and compulsory
measures to overcome patent barriers.
[more]
*******************************************************
A national vaccine effort and speedy rollout is literally a matter of life and death
By Mark Heywood
30 March 2021
Mark Heywood is the editor of Maverick Citizen.
https://www.dailymaverick.co.za/article/2021-03-30-a-national-vaccine-effort-and-speedy-rollout-is-literally-a-matter-of-life-and-death/
Maverick Citizen: Editorial
As South Africa stares at the looming third wave of Covid-19 and the
strong possibility that travel restrictions will be reintroduced over
Easter, it is now clear that the warnings and anger expressed by
scientists and civil society early this year about SA�s vaccine
preparedness were not unfounded.
As of Saturday, we have vaccinated only�220,129 healthcare workers�with the Johnson & Johnson vaccine, as part of the�Sisonke clinical trial. This is about 25% of our health workforce but only 0.4% of our total population. It has not included many front- line workers in the health system, such as community health workers, or administrative staff, such as porters, cleaners and security guards. Vaccines have also not reached rural healthcare workers.
This means that when the third wave breaks, health workers, many of
whom have already been ill with Covid-19, will again find themselves
in the line of danger.
We should be doing much better and people are entitled to honest
answers about why we are failing. It is a matter of life and death.
In developed countries that have scaled up vaccine rollout there is
growing evidence that vaccines are making a difference. For example,
an�editorial�this week in the South African Medical Journal records
that: �Where the AstraZeneca vaccine is in use, mortality in
vaccinated populations has plummeted, including in the UK, home to
its own more infectious and virulent B.1.1.7 variant.�
Questions remain as to why we sold on a million doses of the
AstraZeneca vaccine.
Similarly a�study�just
published in The New England Journal of Medicine has shown that,
after vaccination with the Pfizer and Moderna vaccines, rates of
infection among healthcare workers at California hospitals reduced
the absolute risk of testing positive for SARS-CoV-2 to between 1.19%
and 0.97% among healthcare workers at two large hospitals. Life and
death: these are the reasons why there is growing public anxiety and
anger over South Africa�s failures so far.
There is nothing people in SA want more than unity around a national
vaccine effort. We are desperate to rally behind and contribute to a
well-thought-out national strategic plan, which we are told will soon
be approved by the Cabinet. But to achieve unity government will need
to act differently.
Below are six steps we believe will save lives and restore
confidence.
Consistent reporting of numbers vaccinated and of health system readiness
Since early in 2020 government has released daily reports on the�Coronavirus Resource Portal�of the numbers of Covid-19 infections, tests, deaths and recoveries. It has also sent these reports to the media. This now includes the total number vaccinated. But it is also important that information include numbers of vaccinations by province; by category of health worker; and a list of vaccination sites that are ready for phase two of the rollout.
Publishing all Ministerial Advisory Committee (MAC) advisories
Since 11 January this year�no MAC advisories�have been made public, and in particular none of the advisories of the MAC on Vaccines. People have the right to know what scientists are advising the government and whether government is acting on these advisories.
A high-visibility public communication campaign and community-based social mobilisation to overcome vaccine hesitancy
We are well aware of vaccine hesitancy and misunderstanding. Even nurses are�reported�to be declining vaccinations in some areas. But there is very little visible or audible public information and education campaign. Where there has been information, much of it is on digital platforms, which leaves out millions of people, including those who are most at risk. A massive decentralised campaign in the media, but also on the ground, mobilising the very same people and organisations that will organise the vaccine rollout, needs to start now.
Fixing the health system and rooting out corruption and incompetence
This week Maverick Citizen raised the alarm about the near collapse of the public health system in the Eastern Cape. We�appealed�to the Minister of Health to intervene. Our health system is now in ICU. This threatens our ability to vaccinate and treat not only Covid-19 but also other epidemics of HIV, TB and noncommunicable diseases. There is an urgent need for a fully funded plan to fix the health system. This also means acting against corruption and incompetence that violates constitutional rights, including dignity, life and access to healthcare services.
Transparent negotiations with pharmaceutical companies
So far, we believe, the Vaccine MAC has recommended three vaccines
for use in SA: they are Johnson & Johnson (J&J), Pfizer and Moderna.
Moderna is a highly efficacious vaccine but is excessively priced and
so is not being considered. It is of great concern that negotiations
with AstraZeneca, J&J and Pfizer are taking place in total secrecy.
We have learnt that this is on the instruction of the companies,
which have imposed far-reaching non-disclosure agreements on our
government. This has been their behaviour worldwide. Although it is
accepted that not every aspect of a contractual negotiation can take
place in public, total secrecy causes distrust and fear; it is open
to abuse and corruption. In SA there is a constitutional right of
access to information. Multinational pharmaceutical companies cannot
be allowed to exploit desperation so as to escape public scrutiny
about the terms they are imposing. These private companies have a
monopoly over a public good. South Africa is a sovereign
constitutional state, founded on human rights, and has power in
relation to these companies. Government should be prepared to use it
just as civil society demanded in relation to access to
antiretroviral medicines for HIV.
African and international solidarity and actively pursuing the Trade-Related Aspects of Intellectual Property (TRIPS) waiver
SA and India have formally applied for a waiver of certain provisions
of the World Trade Organisation TRIPS agreement during the course of
the Covid-19 pandemic. Removing ill-deserved intellectual property
barriers could increase the manufacture and supply of Covid-19
vaccines and give governments greater power through the use of
compulsory licensing where warranted. So far SA�s proposal has been
supported by 100 countries, but is being opposed by the US, the UK
and other countries. It is now one year since the start of the hard
lockdown. Perhaps the greatest difference as we enter the second year
is that we now have pharmaceutical interventions that can help us
fight the pandemic.
This is not a reason to dispense with masks, sanitisers or physical
distancing. But it is a means to save lives, limit the damage to our
economy and restore hope. Urgency, transparency and accountability
must start now.
*******************************************************
Links to more recent articles
https://www.pressenza.com/2021/03/why-the-u-s-and-its-allies-are-stupid-to-turn-covid-19-vaccination-into-a-geopolitical-power-play/
https://carnegieendowment.org/2021/02/24/vaccine-geopolitics-could-derail-africa-s-post-pandemic-recovery-pub-83928
https://www.nytimes.com/2021/03/21/world/vaccine-patents-us-eu.html
https://www.washingtonpost.com/business/2021/03/20/covid-vaccine-global-shortages/
https://www.commondreams.org/news/2021/03/12/nobel-economists-suspend-vaccine-patents-halt-pandemic
https://www.washingtonpost.com/opinions/2021/03/10/dont-let-intellectual-property-rights-get-way-global-vaccination/
https://www.theguardian.com/world/2021/mar/30/coronavirus-vaccine-distribution-global-disparity
AfricaFocus Bulletin is an independent electronic publication
providing reposted commentary and analysis on African issues, with
a particular focus on U.S. and international policies. AfricaFocus
Bulletin is edited by William Minter. For an archive of previous Bulletins,
see http://www.africafocus.org,
Current links to books on AfricaFocus go to the non-profit bookshop.org, which supports independent bookshores and also provides commissions to affiliates such as AfricaFocus.
AfricaFocus Bulletin can be reached at africafocus@igc.org. Please
write to this address to suggest material for inclusion. For more
information about reposted material, please contact directly the
original source mentioned. To subscribe to receive future bulletins by email,
click here.
|
